FDA Approves Fourth ALK Inhibitor for Lung Cancer
Last week, a flurry of U.S. Food and Drug Administration (FDA) oncology approvals concluded with the approval of the molecularly targeted therapeutic brigatinib (Alunbrig) for treating certain patients with metastatic non–small cell lung cancer (NSCLC). Specifically, brigatinib is approved for patients who have metastatic NSCLC driven by mutations in the ALK gene and whose disease is not responding to treatment with crizotinib (Xalkori).
Brigatinib and crizotinib are both members of a growing family of molecularly targeted therapeutics called ALK inhibitors. As the name suggests, they work by targeting the signaling protein ALK, which is aberrantly active in 3 to 7 percent of NSCLCs as a result of mutations in the ALK gene.
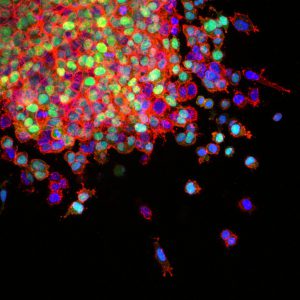
This image shows how lung cancer cells invade surrounding tissues and start to spread. Image courtesy of National Cancer Institute.
Crizotinib was the first ALK inhibitor to be approved by the FDA, in August 2011, and it is now the standard of care for patients with metastatic ALK-positive NSCLC. However, most patients whose NSCLC responds to crizotinib have disease progression within a year of starting treatment because the tumors develop resistance to the anticancer therapeutic.
In many cases, crizotinib resistance emerges because NSCLC cells acquire additional ALK mutations. The next generation of ALK inhibitors to be approved by the FDA, ceritinib (Zykadia) and alectinib (Alecensa), can inhibit most of the clinically observed ALK mutations that drive resistance to crizotinib; these two therapeutics are approved for treating patients with metastatic ALK-positive NSCLC that has either progressed after treatment with crizotinib or has failed to respond to crizotinib in the first place.
The approval of brigatinib for the same indication that ceritinib and alectinib are approved for was based on results from the phase II ALTA clinical trial. According to the FDA announcement, 48 percent of patients who received 90 milligrams (mg) of brigatinib once daily and 53 percent of those who received 180 mg once daily following a 7-day lead-in at 90 mg once daily had complete or partial shrinkage of their tumors.
Because ALK-positive NSCLC frequently metastasizes to the brain and brigatinib was shown to have antitumor activity in a preclinical model of ALK-positive NSCLC metastasis to the brain, researchers looked closely at the effect of brigatinib on brain metastases. Promisingly, the FDA reported that among patients who had measurable brain metastases when they enrolled in the trial, 42 percent and 67 percent of patients in the 90 mg and 180 mg arms, respectively, had complete or partial shrinkage of their brain tumors.
These data are very encouraging, especially for patients whose NSCLC has spread to the brain. However, because the FDA approval was based on objective response rate data, rather than overall survival, brigatinib’s manufacturer, Takeda, is required to conduct a study to confirm that the new ALK inhibitor provides meaningful clinical benefit. Among the clinical trials designed to show this is ALTA 1L, a randomized phase III trial that is comparing brigatinib with crizotinib as a treatment for patients who have not previously received medication to treat ALK-positive NSCLC.
The results of ALTA 1L are eagerly awaited because a key question for oncologists treating patients with ALK-positive NSCLC is: In what order should the four FDA-approved ALK inhibitors be used to provide the maximum benefit for patients?
This question is particularly pertinent given that preclinical studies, which were published recently in the AACR journal Clinical Cancer Research, showed that brigatinib was a more potent in vitro ALK inhibitor than crizotinib, ceritinib, and alectinib and that it could inhibit the clinically observed ALK mutations that drive resistance to the three previously approved ALK inhibitors.
Several other ongoing phase III clinical trials will help shed light on this issue, including the ASCEND-4 clinical trial, which was recently reported to have shown that ceritinib more than doubled the median progression-free survival for patients who have not previously received medication to treat advanced ALK-positive NSCLC compared with chemotherapy, and the ALEX clinical trial, which Roche recently announced met its primary endpoint and showed that median progression-free survival was significantly longer among people treated with alectinib than among those treated with crizotinib.



